On her drive to work, Rachel caught her reflection in the rearview mirror and paused. Her upper canine looked “longer” than last year, and a sip of iced coffee sent a quick sting through the spot where the gum had crept up. She started brushing more (harder, if we’re honest), then switched to a whitening toothpaste hoping the color would distract from the new shape. Nothing changed—except the sensitivity. If this sounds familiar, you’re not alone. Gum recession is surprisingly common, and when it exposes root surfaces, a gum graft—also called soft-tissue grafting—can restore coverage, comfort, and confidence.

Our job in this guide is to translate the process into clear, patient-first language so you can decide when it’s time to act, what recovery really feels like, and how we keep treatment gentle at our Highland office.
Why Gums Recede in the First Place
Sometimes recession is slow and quiet; other times it appears quickly after orthodontics, a lip or tongue piercing, or months of enthusiastic brushing with a stiff bristle. Genetics also plays a role—some people simply inherit thinner, more delicate gum tissue. Inflammation from plaque, clenching or grinding forces, and tobacco can all nudge the margin downward over time.
Two things matter most:
- Tissue thickness: Thin gums are easier to irritate and reposition.
- Bone support: If the tooth sits just outside the bony “housing,” the gum has less to hold onto.
A gum graft doesn’t just cover a bare root like a bandage. It adds thickness where you need it, which is the key to long-term stability.
What A Gum Graft Actually Does
A gum graft replaces thin, receded gum with new tissue so it can cover exposed root, reduce sensitivity, and better resist future recession.
There are a few ways to do it. We may borrow a small layer of your own tissue from the palate, use carefully processed donor tissue (avoiding a second site), or gently advance nearby gum over the exposed area and support it with a thin graft underneath. The best choice depends on which tooth we’re treating, how you smile, and how much thickness you need to stay stable for the long haul.
Do You Really Need One?
You don’t need surgery for every bit of recession. The decision comes down to three questions:
- Is the root exposed and sensitive? If cold air, water, or brushing zings the area, coverage helps.
- Is the margin still moving? Progressive recession—even without pain—puts the tooth at risk.
- Is this a front-and-center tooth? A graft can protect structure and keep your smile line even.

If your gums bleed easily or feel puffy, we’ll calm things first—often with scaling and root planing—then re-measure. Healthy, quiet tissue heals better and gives your graft the best start.
What Your Visit Looks Like
A smooth experience starts with clarity. At Fortson Dentistry, we measure—not guess—so your plan fits your anatomy and your goals.
Consult & planning
We begin with a conversation and photos, then check gum thickness and root shape. When needed, a small 3-D scan helps us map the area with precision. You’ll see exactly which tooth (or teeth) would benefit, why, and what kind of tissue we’ll use.
Comfort strategy
You’ll be fully numb. If you’re anxious or simply want a calmer appointment, we offer sedation dentistry. Patients often say the visit felt shorter than expected.
The procedure
We gently prepare the site, place the tissue, and secure it with fine sutures. If we borrow a small layer from the palate, you’ll leave with a slim protective stent so eating and speaking feel normal.
Aftercare
You’ll get a simple, one-page plan: how to rinse, what to eat for the first few days, and when to return. Most people go back to work the next day.
How Recovery Really Feels
Think “tender,” not “trauma.” The gum near the graft can feel like a bruise for a few days; over-the-counter relief and cool, soft foods are usually all that’s needed. If we used the palate, the protective stent is a game-changer—you’ll barely notice it after day two. Most swelling is mild and fades quickly.
What you’ll do:
- Avoid pulling your lip to “peek.” (It tugs the sutures.)
- Rinse as directed; brush carefully around—not on—stitches for the first week.
- Shift to fork-and-knife foods for a few days; skip spicy or very hot foods early on.
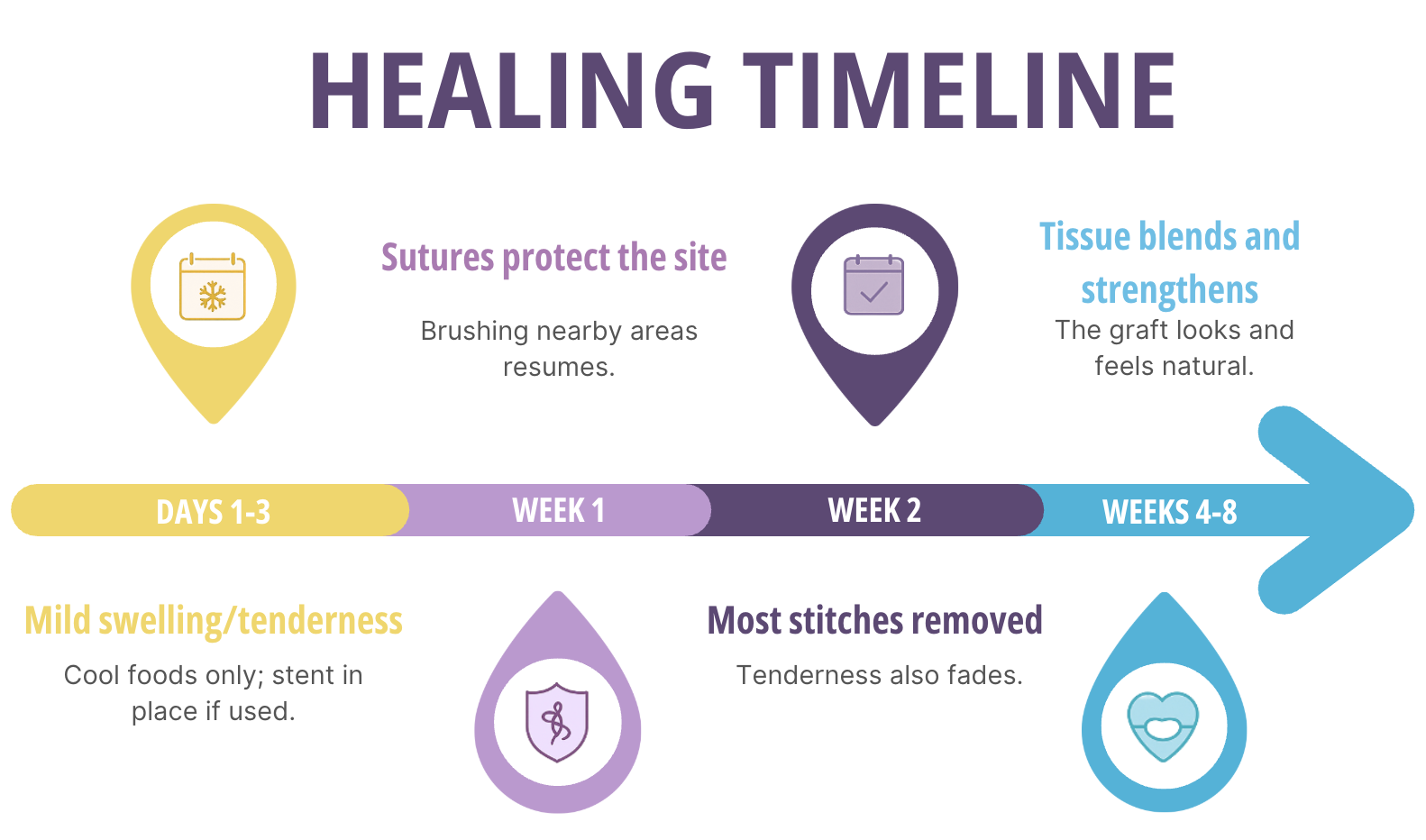
Comfort, Confidence, and The Way It Looks
Front-tooth grafts are planned with your smile in mind—where your lip rests, how your gum scallops, and how the tissue should blend under bright light. Connective-tissue grafts (using your tissue) often give the most seamless match at the front; donor tissue shines when multiple teeth need help or you’d like one healing site instead of two. Either way, the goal is natural: gums that don’t call attention to themselves, but quietly support a beautiful tooth shape.

A Quick Word on Bone Health
Recession rides on the surface, but bone support beneath the gum is what keeps the margin steady. Heavy clenching or grinding can thin the bone and strain delicate tissue. If we see signs of wear, we’ll recommend a custom night guard to spread bite forces and protect your new graft. It’s a small step that pays long-term dividends.







.png)